Medications
Usually prescribed by experimentation Starts on a low-dose, and moves up from there
Evidenced Based Intervention
Evidence-based interventions for depression are therapeutic practices or programs that have been proven effective through rigorous research and evaluation. These interventions are grounded in empirical evidence, clinical expertise, and patient characteristics.
In the context of depression treatment, evidence-based practice (EBP) aims to optimize the effectiveness of therapeutic interventions. It encourages therapists to use the best available research evidence to make informed decisions about patient care.
The American Psychological Association defines evidence-based practice in psychotherapy as “the integration of the best available research with clinical expertise in the context of patient characteristics, culture, and preferences”. This means therapists should use their professional judgment to make collaborative decisions with the patient based on the best clinically relevant evidence. They should consider the probable costs and benefits of different treatments, available resources, and the patient’s preferences.
In the field of mental health, evidence-based methods and interventions have been proven effective. The effects are clearly linked to the activities themselves, not to outside, unrelated events.
A typical evidence-based intervention for depression might include value-finding exercises. Identifying what matters to the patient and what they want their life to be about can positively impact well-being and help manage depression. Other evidence-based interventions for depression might include cognitive-behavioral therapy (CBT), interpersonal therapy (IPT), and certain types of medication. These treatments have been shown to be effective in reducing symptoms of depression and improving quality of life.
CBT
Cognitive Behavioral Therapy (CBT) is a widely used and effective treatment for depression1. It’s a type of psychotherapy that uses a combination of cognitive and behavioral approaches to reduce depression2. Here’s how it works:
- Identify and Challenge Negative Thoughts: CBT helps you spot and challenge automatic negative thoughts linked to depression, like feeling helpless, hopeless, or worthless1.
- Restructure Cognitive Patterns: A therapist will work with you to reframe your interpretation of life events, altering any core beliefs that contribute to depressive symptoms1.
- Develop Coping Strategies: CBT teaches effective coping skills and problem-solving techniques to handle challenging situations1.
- Behavioral Activation: Your CBT therapist will encourage you to do enjoyable things to fight against feeling withdrawn and inactive, common feelings in depression1.
- Relapse Prevention: CBT not only treats current symptoms but also focuses on preventing future relapses by teaching strategies to maintain healthier thoughts and behavior patterns1.
CBT can be an effective treatment for various depressive disorders and episodes that may be impacting your life, especially in the mild to moderate range of symptoms2. These include Major Depressive Disorder (clinical depression), Persistent Depressive Disorder (PDD), Seasonal Affective Disorder, Postpartum Depression, the depressive episodes of Bipolar Disorder, Situational Depression, and Schizoaffective Disorder, depressive type2.
Studies demonstrate that combining CBT with medication is more effective than medication alone, and individuals undergoing CBT experience reduced relapse rates1. Even after therapy concluded, the benefits persisted1.
It’s important to note that the effectiveness of CBT can depend on the individual’s willingness to participate actively, their ability to identify their emotions, their preference for non-medication approaches, and their commitment to regular therapy sessions1.
Understanding Emotions
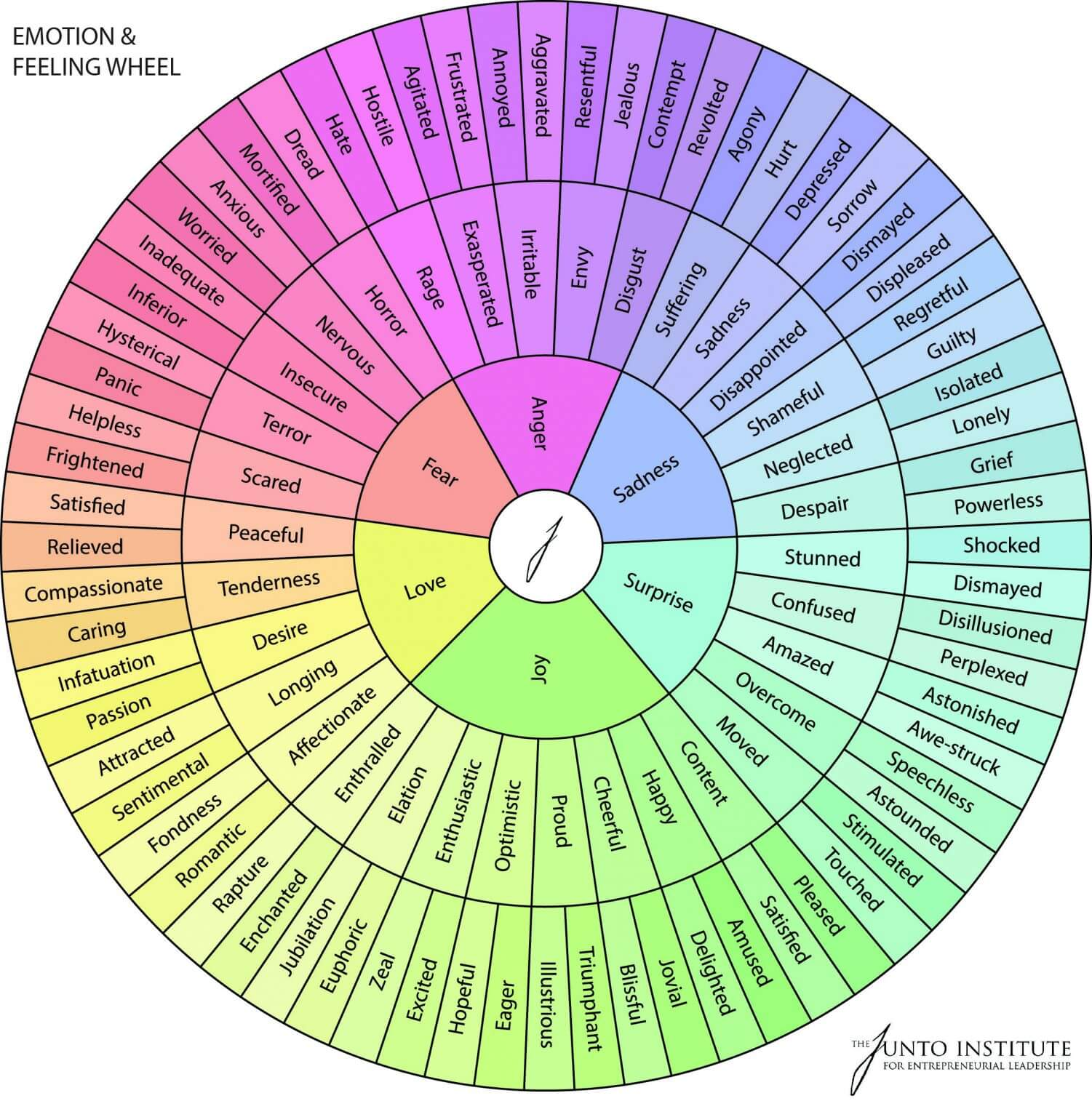
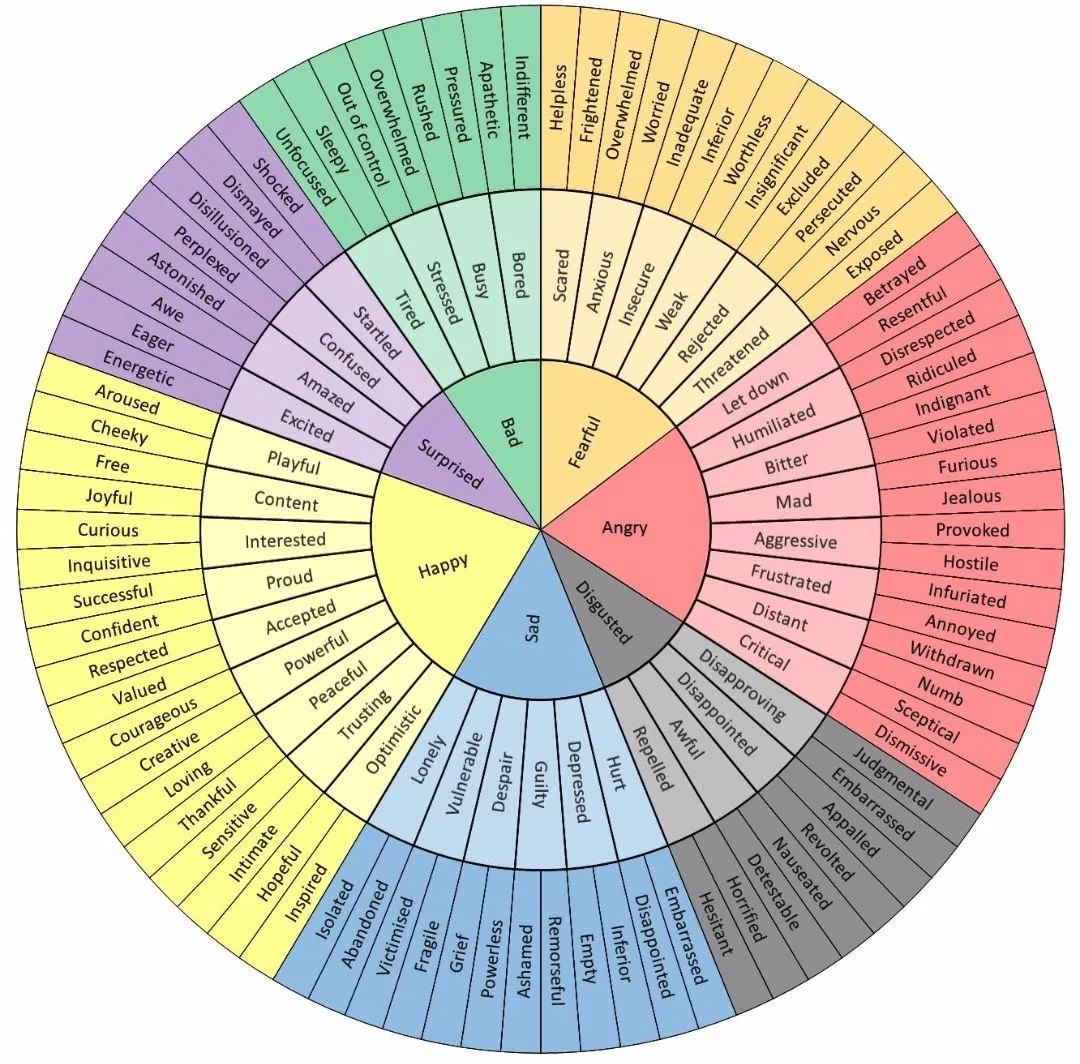
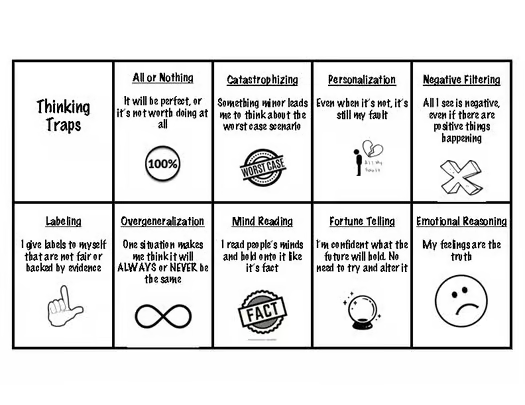
Thinking Traps